A Rational, Health-Centered Approach to Psoriasis Management
Introduction
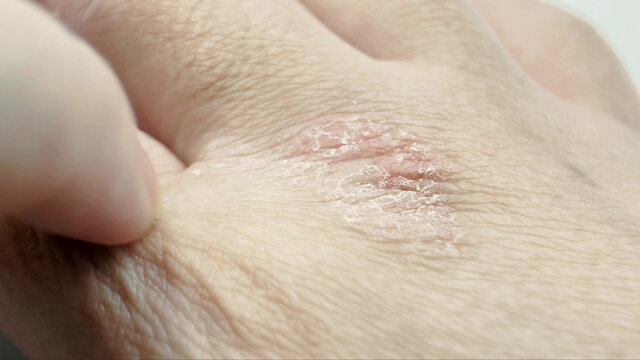
Psoriasis is a chronic, immune-mediated skin disease affecting 2–3% of the population worldwide. Characterized by sharply demarcated plaques with silvery scales, psoriasis imposes a substantial burden on physical health and psychosocial well-being. Traditional “disease-centered” strategies focus narrowly on keratinocyte hyperproliferation and symptom suppression, often overlooking the patient’s holistic health. This article synthesizes international consensus and emerging concepts advocating a “health-centered,” collaborative, and evidence-based framework for rational psoriasis management.
- Introduction
- 1. International Consensus: Tenets for Patient and Clinician
- 2. Psychosomatic Dimensions of Psoriasis
- 3. Health-Centered vs. Disease-Centered Paradigms
- 4. Collaborative Doctor-Patient Partnership
- 5. Medication Stewardship and Avoiding Drug Abuse
- 6. Shao Changgeng-Yang Xueqin’s Rational Treatment Concept
- 7. Integrating New Therapies
- Conclusion
1. International Consensus: Tenets for Patient and Clinician
At the 2003 International Psoriasis Council meeting, experts agreed on ten principles to guide care:
1. Immune-Mediated Disease: Psoriasis is driven by dysregulated skin and systemic immune pathways, not infectious contagion.
2. Universal Prevalence: All races, genders, and age groups are susceptible; pediatric and adult-onset variants exist.
3. Non-Communicable: Patients do not transmit disease; stigma should be addressed.
4. Variable Severity: Disease ranges from localized plaques to erythroderma; treatments must be individualized.
5. No Universal Cure: Multiple therapies exist, but no single modality works for every patient.
6. Treatment Risks: Systemic agents carry significant side effects; cost and safety impact quality of life.
7. Natural Cycle: Psoriasis may flare and remit; long-term strategies should anticipate variability.
8. Psychosocial Impact: Anxiety, depression, and social withdrawal are common—mental health support is essential.
9. Discrimination and Stigma: Public misunderstanding contributes to patient isolation.
10. Education and Empowerment: Informed patients and clinicians partnering in care yield better outcomes.
These principles underscore the need for comprehensive, patient-centered approaches rather than quick-fix regimens.
2. Psychosomatic Dimensions of Psoriasis
Psoriasis exemplifies a psychosomatic disorder: stress, mood disturbances, and personality traits (Type A behavior) can precipitate or exacerbate flares. Research highlights:
– Neuroimmune Markers: Elevated local expression of heat-shock proteins, nerve growth factors, and systemic stress mediators correlate with disease activity.
– Stress-Reduction Interventions: Biofeedback, relaxation training, and cognitive-behavioral therapy have demonstrated efficacy in decreasing lesion severity and reducing reliance on pharmacotherapy.
Clinical takeaway: Screening for psychological stress and integrating behavioral interventions can significantly enhance treatment response and patient resilience.
3. Health-Centered vs. Disease-Centered Paradigms
- Disease-Centered Model: Prioritizes rapid plaque clearance through high-potency topical steroids or systemic immunosuppressants, often at the expense of systemic balance and patient quality of life.
- Health-Centered Model: Emphasizes overall well-being—addressing nutrition, comorbid conditions (e.g., metabolic syndrome), mental health, and lifestyle factors while targeting skin pathology with the least toxic effective therapies.
Implementation:
– Incorporate dietary counseling, smoking cessation, and weight management.
– Use the lowest effective dose of systemic agents, combine with phototherapy or biologics when indicated, and monitor for adverse effects.
4. Collaborative Doctor-Patient Partnership
Effective psoriasis care requires co-management:
– Comprehensive Assessment: Evaluate disease severity (PASI, BSA), comorbidities (cardiovascular risk, psoriatic arthritis), psychosocial factors, and treatment goals.
– Shared Decision-Making: Discuss benefits, risks, and real-world considerations (cost, access, lifestyle) of each therapy.
– Self-Management Education: Teach proper topical application, phototherapy protocols, and relapses early-warning signs.
– Regular Follow-Up: Adjust treatment plans based on objective metrics and patient-reported outcomes (DLQI, POEM).
5. Medication Stewardship and Avoiding Drug Abuse
Unsupervised polypharmacy and overreliance on potent topical or systemic agents can trigger adverse events:
– Quack Remedies: Unregulated antileukemic or mercury-containing preparations cause systemic toxicity.
– Herbal and OTC Overuse: Can worsen psoriasis via irritant contact or drug interactions.
– Overtreatment: Prolonged high-dose corticosteroids lead to HPA axis suppression and skin atrophy.
Best practices:
– Verify all concurrent medications and supplements.
– Educate patients about credible information sources.
– Adhere to guideline-based dosing and taper protocols.
6. Shao Changgeng-Yang Xueqin’s Rational Treatment Concept
In the 2006 monograph Research on the Prevention, Treatment, and Rational Treatment of Psoriasis, Shao and Yang introduce “Knowledge-Based Medical Care, Green Treatment,” stressing:
– Rational Pharmacotherapy: Use targeted therapies judiciously to minimize systemic burden.
– Holistic Health Focus: Prioritize psychological well-being, lifestyle optimization, and patient empowerment.
– Prevention of Iatrogenic Harm: Avoid toxic agents and excessive immunosuppression.
This framework aligns with modern precision medicine principles—tailoring therapy to individual risk profiles and health objectives.
7. Integrating New Therapies
The therapeutic landscape has evolved with biologics and small molecules:
– Biologics targeting TNF-α, IL-17, IL-23, and IL-12/23 offer durable clearance with favorable safety compared to conventional immunosuppressants.
– JAK Inhibitors and PDE4 inhibitors provide oral options for moderate-to-severe disease.
– Emerging Agents: Anti-IL-36 for pustular forms, novel topical tyrosine-kinase inhibitors under investigation.
Rational use:
– Reserve high-cost therapies for patients with moderate-to-severe disease or significant comorbidity.
– Monitor infection risk, laboratory parameters, and long-term safety data.
Conclusion
A rational, health-centered approach to psoriasis integrates international consensus, psychosomatic insights, collaborative care models, and judicious pharmacotherapy. By prioritizing overall patient health, minimizing harm, and harnessing modern targeted therapies, clinicians can achieve sustained disease control and improve quality of life for individuals living with psoriasis.