Joint Dislocation: Clinical Guide for Health Professionals
Introduction
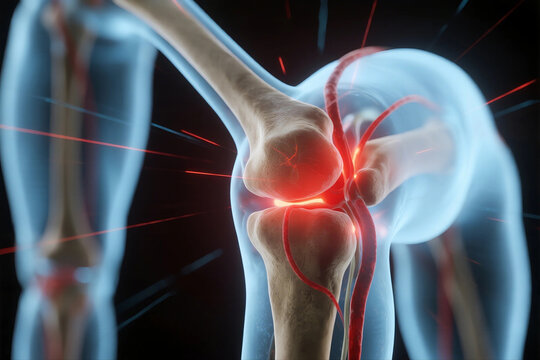
A joint dislocation is the loss of normal congruity between articular surfaces, often accompanied by ligamentous, capsular, and soft tissue injury. Dislocations range from partial (subluxation) to complete separations and may be acute or chronic. Timely recognition, appropriate reduction, neurovascular assessment, and structured rehabilitation are essential to minimize complications and restore function.
Common Sites and Etiology
- Shoulder (glenohumeral): The most frequently dislocated major joint; anterior dislocations predominate following forced abduction and external rotation.
- Elbow: Often from a fall on an outstretched hand with the elbow in extension; posterior elbow dislocations are common.
- Hip: High-energy trauma (e.g., motor vehicle collisions) may produce posterior hip dislocation; urgent reduction is required.
- Patellofemoral: Lateral patellar dislocation often occurs in young athletes.
- Digit and small joint dislocations: Common in sports and manual activities.
- Other: Sternoclavicular and temporomandibular joint (TMJ) dislocations have distinct considerations.
Initial Assessment (On Presentation)
- Primary survey: Address life‑threatening injuries first in polytrauma.
- Focused musculoskeletal exam: Inspect for deformity, swelling, skin tenting, open wounds, and check active/passive range of motion where feasible.
- Neurovascular assessment: Palpate distal pulses, compare capillary refill, and perform detailed motor and sensory testing of the limb—document findings before and after any intervention.
- Imaging: Obtain appropriate radiographs (AP/lateral/axial or dedicated views) to confirm dislocation, determine direction, and identify associated fractures. CT is useful for complex or acetabular/hip injuries; MRI is reserved for soft-tissue assessment when needed.
Principles of Management
The management of joint dislocation follows three core principles: prompt and safe reduction, appropriate immobilization, and structured rehabilitation.
Reduction
- Urgency: Major joint dislocations with compromised neurovascular status or hip dislocations require urgent reduction—ideally within 6 hours for hip dislocations to reduce the risk of avascular necrosis.
- Analgesia and relaxation: Use procedural sedation, regional nerve blocks, or adequate analgesia to facilitate muscle relaxation and safe reduction.
- Technique: Choose a reduction maneuver appropriate to the joint (e.g., Kocher or traction-countertraction for anterior shoulder dislocation; Stimson, Milch, or scapular manipulation as alternatives). For elbow dislocation, gentle longitudinal traction with flexion is commonly employed. For patellar dislocation, reduction is often achieved with gentle medial pressure and extension of the knee.
- Fracture-dislocations: Avoid forceful closed reduction if a significant associated fracture is suspected—consult orthopedics for possible open reduction.
Post-reduction Care
- Immediate reassessment: Repeat neurovascular exam and document any change.
- Post-reduction imaging: Radiographs to confirm successful reduction and to identify occult fractures; CT if concern persists.
- Wound care: For open dislocations, administer appropriate antibiotics and tetanus prophylaxis and consult surgery for debridement.
Immobilization and Timing
- Duration: Immobilization time varies by joint and injury severity—shoulder immobilizers or slings commonly for 2–4 weeks; elbow in posterior splint at ~90° for 1–3 weeks; patellar bracing and support, followed by early mobilization to prevent stiffness.
- Type: Choose an immobilizer that maintains reduction while minimizing stiffness; consider hinged braces when early controlled motion is indicated.
Rehabilitation and Functional Recovery
- Early controlled mobilization: Once soft tissues tolerate it, begin guided range-of-motion and progressive strengthening to restore dynamic stability and proprioception.
- Physiotherapy goals: Pain control, edema management, restoration of range of motion, rotator cuff and scapular stabilization for shoulder injuries, and quadriceps/hamstring strength recovery for knee/patellar injuries.
- Return-to-play/work: Tailored to joint, severity, and occupational demands; emphasize gradual progression and objective functional testing.
Complications and Red Flags
- Neurovascular injury: Persistent paresthesia, absent pulses, or worsening ischemia after reduction mandate immediate re-evaluation and vascular/orthopedic consultation.
- Associated fractures: May require internal fixation to restore joint congruity.
- Chronic instability: Recurrent dislocations (e.g., shoulder) may necessitate surgical stabilization (e.g., Bankart repair, Latarjet procedure).
- Post-traumatic arthritis and stiffness: Particularly after intra-articular fractures or delayed reduction.
- Avascular necrosis: Particularly concerning in hip dislocations; risk increases with delay to reduction.
Special Considerations by Joint
- Shoulder: Young, active patients with first-time dislocation have high recurrence risk—consider early specialist referral for high-risk athletes. Immobilization position (internal vs external rotation) is controversial; emphasize early scapular and rotator cuff rehabilitation.
- Elbow: Beware of neurovascular compromise (brachial artery, median and ulnar nerves) and the risk of heterotopic ossification—avoid aggressive passive stretching early.
- Hip: Posterior dislocations often present with shortened, internally rotated limb—reduce emergently and monitor for AVN with serial imaging.
- TMJ: Acute anterior dislocation is often reduced manually with downward and posterior pressure on the mandible; advise soft diet and avoid wide mouth opening during recovery.
Disposition and Follow-up
- Outpatient follow-up: Orthopedic or sports medicine review within 1–2 weeks to evaluate healing and plan rehabilitation.
- Indications for admission: Open dislocation, vascular injury, polytrauma, inability to achieve reduction in the ED, or need for operative management.
- Patient education: Discuss activity modification, signs of neurovascular compromise, wound care, and the importance of adherence to physiotherapy.
Conclusion
Joint dislocations are common and spectrum-spanning injuries. Management hinges on prompt recognition, safe reduction, meticulous neurovascular assessment, appropriate immobilization, and progressive rehabilitation. Early specialist involvement is essential for complex injuries, fractures, recurrent instability, or neurovascular compromise to optimize long-term function and minimize complications.