Introduction
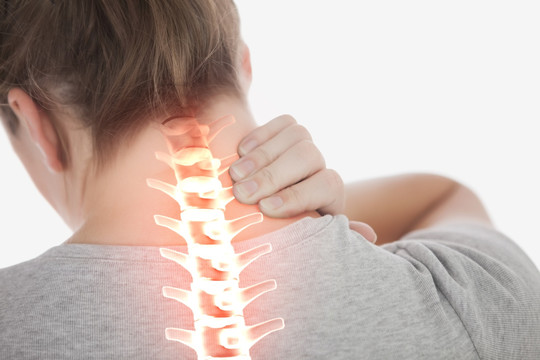
Cervical spondylosis is a prevalent, age-related degenerative disorder of the cervical spine characterized by intervertebral disc desiccation, osteophyte formation, and ligamentous hypertrophy. While many adults exhibit radiographic changes, only a subset becomes symptomatic, presenting with pain, neurological deficits, or vascular compromise. An evidence-based, multidisciplinary approach is essential to optimize functional recovery, minimize complications, and enhance quality of life.
- Introduction
- Epidemiology and Risk Factors
- Pathophysiology
- Clinical Presentation
- 1. Axial Neck Pain
- 2. Cervical Radiculopathy
- 3. Cervical Myelopathy
- 4. Vertebrobasilar Insufficiency and Autonomic Features
- Diagnostic Evaluation
- Differential Diagnosis
- Conservative Management
- Surgical Management
- Rehabilitation and Follow-Up
- Patient Education and Prevention
- Conclusion
Epidemiology and Risk Factors
- Prevalence: Radiographic signs appear in over 85% of individuals aged 60 and above; symptomatic disease affects approximately 10–20% of this population.
- Age and Sex: Incidence increases with age; both sexes are equally affected, though men may present earlier with radiculopathy.
- Genetic and Environmental Factors: Family history, repetitive neck motion, poor posture, smoking, and history of cervical trauma accelerate degenerative changes.
Pathophysiology
Degeneration initiates in the intervertebral disc with loss of hydration and proteoglycan content, reducing disc height and shifting mechanical load to facet joints and uncovertebral regions. Subsequent osteophyte development and ligamentum flavum hypertrophy narrow the spinal canal and neuroforamina. Compression or irritation of nerve roots, spinal cord, or vertebrobasilar arteries precipitates the clinical syndrome.
Clinical Presentation
1. Axial Neck Pain
- Dull, chronic ache localized to the posterior neck with radiation to the trapezius or scapular regions.
- Exacerbated by prolonged static posture (e.g., desk work) and alleviated by movement or heat.
2. Cervical Radiculopathy
- Dermatomal pain distribution, commonly C6 (lateral forearm and thumb) and C7 (posterior arm and second digit).
- Paresthesia and sensory loss in affected dermatomes; motor weakness manifesting as decreased elbow flexion, wrist extension, or grip strength.
- Positive Spurling’s maneuver reproducing radicular symptoms.
3. Cervical Myelopathy
- Gait instability, clumsy hand use, and fine motor deficits (e.g., buttoning clothes).
- Hyperreflexia, Hoffmann’s sign, Babinski’s sign, and Lhermitte’s phenomenon may be present.
- In advanced cases, urinary urgency or retention indicates significant cord involvement.
4. Vertebrobasilar Insufficiency and Autonomic Features
- Dizziness, vertigo, diplopia, tinnitus, and ataxia due to transient vertebral artery compromise during neck extension.
- Headaches, diaphoresis, and palpitations suggesting sympathetic chain irritation.
Diagnostic Evaluation
- History and Physical Exam: Focused neurologic assessment including motor strength grading, sensory mapping, reflex testing, and gait analysis.
- Plain Radiography: Anteroposterior, lateral, and flexion-extension views to evaluate alignment, disc height, osteophytes, and dynamic instability.
- Magnetic Resonance Imaging (MRI): Gold-standard for soft tissue visualization—disc herniation, ligamentous hypertrophy, and cord signal changes.
- Computed Tomographic Myelography: Consider when MRI is contraindicated or to refine preoperative planning of bony anatomy.
- Electrodiagnostic Studies: Electromyography (EMG) and nerve conduction studies (NCS) differentiate radiculopathy from peripheral neuropathy.
Differential Diagnosis
- Rotator cuff pathology
- Thoracic outlet syndrome
- Peripheral neuropathies (e.g., carpal tunnel syndrome)
- Central nervous system disorders (e.g., multiple sclerosis)
Conservative Management
Conservative therapy remains first-line for mild to moderate cases without significant myelopathy.
– Physical Therapy: Emphasize posture correction, cervical traction, mobilization exercises, and scapular stabilization.
– Pharmacotherapy: NSAIDs as first-line analgesics; short courses of muscle relaxants for acute spasm; neuropathic agents (e.g., gabapentin) for radicular pain.
– Activity Modification: Ergonomic adjustments, frequent breaks from repetitive tasks, and avoidance of extreme neck extension or flexion.
– Support Devices: Soft cervical collars for short-term pain relief (<2 weeks) to limit motion without causing deconditioning.
– Interventional Procedures: Fluoroscopically guided epidural steroid injections and facet joint blocks for refractory radicular or axial pain.
Surgical Management
Surgical consultation is warranted for patients with progressive myelopathy, refractory radiculopathy, or radiographic cord compression with neurologic deficits.
– Anterior Cervical Discectomy and Fusion (ACDF): Decompression via discectomy, interbody graft placement, and anterior plating. High fusion rates and reliable symptom relief.
– Cervical Disc Arthroplasty: Motion-preserving alternative in select patients, reducing adjacent segment degeneration risk.
– Posterior Decompression and Fusion: Laminectomy with or without instrumented fusion for multilevel stenosis, particularly when anterior approach is contraindicated.
Rehabilitation and Follow-Up
- Initiation of postoperative physical therapy focusing on gentle range-of-motion exercises, isometric strengthening, and postural training.
- Serial imaging at 3, 6, and 12 months to assess hardware position, fusion status, and adjacent segment changes.
- Long-term surveillance for adjacent segment disease in fusion patients; address modifiable risk factors to delay progression.
Patient Education and Prevention
- Ergonomics: Chair height, monitor position at eye level, and supportive pillows for sleep.
- Exercise: Daily neck stretching, scapular strengthening, and regular cardiovascular exercise to promote spinal health.
- Lifestyle Modifications: Smoking cessation, weight management, and optimal bone health (adequate calcium and vitamin D intake).
- Symptom Awareness: Educate on red-flag signs such as new-onset limb weakness, gait disturbance, or urinary dysfunction that require urgent evaluation.
Conclusion
Cervical spondylosis encompasses a spectrum of degenerative changes with potential neurologic and vascular sequelae. A structured, stepwise approach—beginning with conservative management, timely diagnostics, and appropriate surgical referral—optimizes patient outcomes. Multidisciplinary collaboration and patient engagement in ergonomics and exercise are pivotal in mitigating long-term disability and preserving cervical spine function.